Connection
How social safety and community shape nervous system health
For many people, wellness begins with a simple observation: I feel better.
After time in a sauna, a cold plunge, a yoga class, or a quiet moment of breathwork, there is often a noticeable shift—less tension, more clarity, a sense of ease. These experiences matter. But feeling better is only the first step. The deeper question is:
What is happening in the body—and how does that translate into long-term health and longevity?
This is where connection becomes clinically relevant.
Connection Is a Biological Input
Connection is often described as emotional or psychological. Increasingly, research demonstrates that it functions as a biological signal of safety.
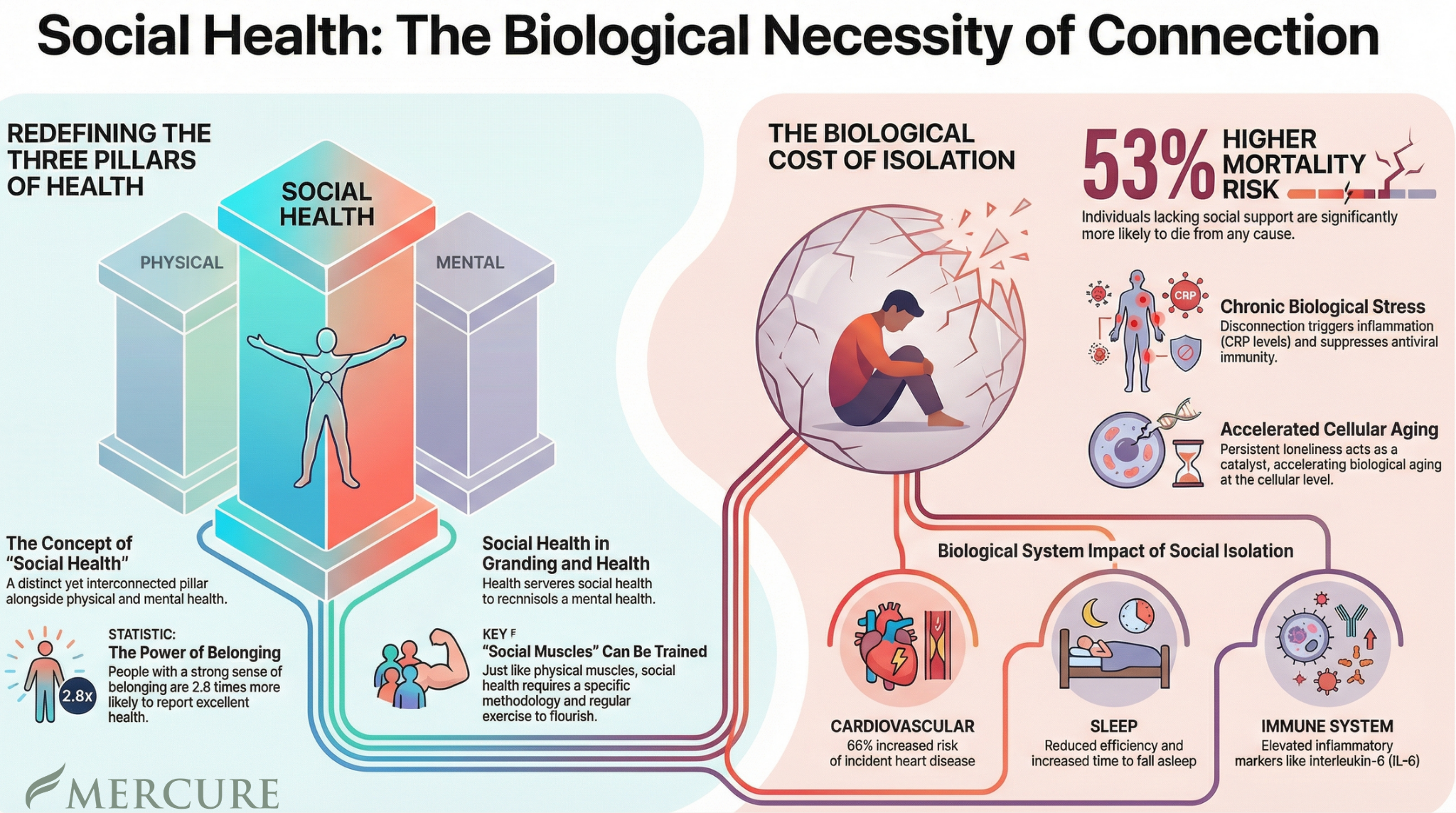
Large meta-analyses show that social isolation is associated with significantly increased all-cause mortality risk¹, and persistent loneliness over time carries even greater risk². Prolonged social disconnection has also been linked to accelerated biological aging at the cellular level² and increased cardiovascular disease risk¹¹.
These findings are not abstract. They indicate that the body interprets social conditions as meaningful inputs that influence survival systems.
Connection is not simply comforting.
It is regulatory.
The Nervous System Bridge: Safety vs. Threat
The nervous system constantly evaluates whether the environment is safe enough for repair.
When social safety is present—through trusted relationships, shared experience, or predictable community—the nervous system shifts out of vigilance. Energy can then be allocated toward:
Immune regulation
Tissue repair
Hormonal balance
Sleep consolidation
Adaptive resilience
When isolation or chronic loneliness is present, the system tends to prioritize protection. This state is associated with:
Elevated inflammatory markers such as CRP and IL-6⁶⁷
Dysregulation of the HPA axis and altered cortisol rhythms⁷
Increased allostatic load (cumulative stress burden)¹⁸
Poorer sleep efficiency and longer sleep latency¹⁴¹⁵
Importantly, these relationships are bidirectional. Inflammation predicts future loneliness, and loneliness predicts future inflammation⁸. Poor sleep increases loneliness, and loneliness worsens sleep¹⁶¹⁷.
Connection, therefore, operates as a nervous system signal that influences multiple biological systems simultaneously.
Social Health: The Biological Necessity of Connection
From Feeling Better to Progressing
Many wellness practices support the nervous system directly—heat exposure, breathwork, movement, and restorative environments all provide physiological inputs that reduce threat signaling.
However, without consistent social support, the system may struggle to sustain progress.
Adaptation follows support—not effort alone.
Social safety reduces baseline stress load. When that load decreases, the body becomes more responsive to exercise, recovery, nutrition, and medical optimization. In this way, connection acts as a multiplier for other longevity practices.
System-Level Impacts of Social Disconnection
Research demonstrates that social isolation influences the same systems targeted by most longevity interventions:
Cardiovascular System
Lack of social support and social isolation significantly increase cardiovascular disease risk¹¹. In older adults, social isolation has been associated with a 66% increased risk of incident cardiovascular disease¹².
Immune & Inflammatory Pathways
Social adversity increases inflammatory signaling while suppressing antiviral immunity⁹. Over time, chronic inflammation contributes to cardiometabolic disease development.
Encouragingly, psychosocial interventions have been shown to improve immune function, with pooled effects across randomized trials demonstrating measurable enhancement¹⁰.
Sleep Architecture
Loneliness is consistently associated with longer sleep latency, more awakenings, and reduced sleep efficiency¹⁴¹⁵. Sleep and loneliness reinforce each other in a reciprocal cycle¹⁶¹⁷.
Biological Aging
Persistent loneliness and social isolation are associated with markers of advanced biological aging².
These findings reinforce a central idea:
Connection influences the same biological pathways that determine how we age.
Practical Ways to Strengthen Support
Connection does not require dramatic gestures.
Small, predictable signals of support are often more regulating than large, infrequent efforts.
One practical approach is to reduce decision fatigue around outreach. Writing the names of trusted friends or family members on slips of paper and placing them in a bowl allows connection to become routine rather than effortful. Once or twice per week, drawing a name and sending a brief message creates consistent nervous system signals of safety.
Pairing connection with supportive environments—movement classes, recovery practices, shared wellness experiences—can further reinforce physiological regulation.
Support is received by the body, not decided by willpower.
Longevity Begins With Conditions the Body Can Trust
Longevity is not simply about extending lifespan. It is about preserving recovery capacity, adaptability, and resilience.
When the body feels supported—socially, physiologically, environmentally—it can invest in repair instead of protection.
Connection is not separate from health optimization.
It is foundational to it.
A Clinical Next Step
For some individuals, persistent stress, sleep disruption, hormonal imbalance, or inflammatory markers may indicate that additional support is needed beyond behavioral adjustments.
A functional medicine consultation can help evaluate laboratory markers, hormonal status, inflammatory indicators, and sleep-related contributors that may be influencing nervous system regulation.
If you’re interested in exploring medical optimization strategies alongside lifestyle support, you can learn more here:
👉 Hormone Optimization & Functional Medicine Services
Support does not have to be guesswork. It can be evaluated, measured, and strengthened.
References
Naito R, et al. PLOS One. 2023.
Crowe CL, et al. J Gerontology A. 2021.
Smith KJ, et al. Neurosci Biobehav Rev. 2020.
Zilioli S, Jiang Y. Psychoneuroendocrinology. 2021.
Gao Q, et al. Brain Behav Immun. 2024.
Leschak CJ, Eisenberger NI. Psychosom Med. 2019.
Shields GS, et al. JAMA Psychiatry. 2020.
Liu Z, et al. Soc Psychiatry Psychiatr Epidemiol. 2025.
Freak-Poli R, et al. BMC Geriatr. 2021.
Benson JA, et al. Sleep. 2021.
Peng A, et al. Sleep Med. 2021.
Dickman KD, et al. Psychosom Med. 2024.
Dworschak C, et al. Sci Rep. 2024.
Larrabee Sonderlund A, et al. PLOS One. 2019.